Rise in jail deaths is especially troubling as jail populations become more rural and more female
New data show record high deaths of people locked up in jail, as jail populations have shifted toward smaller, rural jails and growing numbers of women. A lack of accountability and acknowledgement of women’s unique disadvantages all but ensures more deaths to come.
by Leah Wang, June 23, 2021
In so many communities nationwide, jails act as reception centers for those experiencing poverty, mental health crises, or substance use disorders. Just a few days ago, Representative Alexandria Ocasio-Cortez referred to jails as “garbage bins for human beings.” This statement tracks with new data that show that even before the COVID-19 pandemic, deaths in jail had reached record high numbers, because they continue to be unregulated, under-resourced places where disadvantaged people are sent to languish.
The Bureau of Justice Statistics (BJS) recently came out with the 2018 mortality data for local jails. Nationwide, there were 1,120 deaths reported, or a rate of 154 deaths per 100,000 people in jail, the highest levels since BJS’ first report on this topic in 2000. The jail population has grown since 2000, of course, but jail deaths have grown more. These deaths spared no demographic, and almost no state; more jurisdictions than ever reported one or more deaths in 2018.
Dying in jail often happens within days or weeks
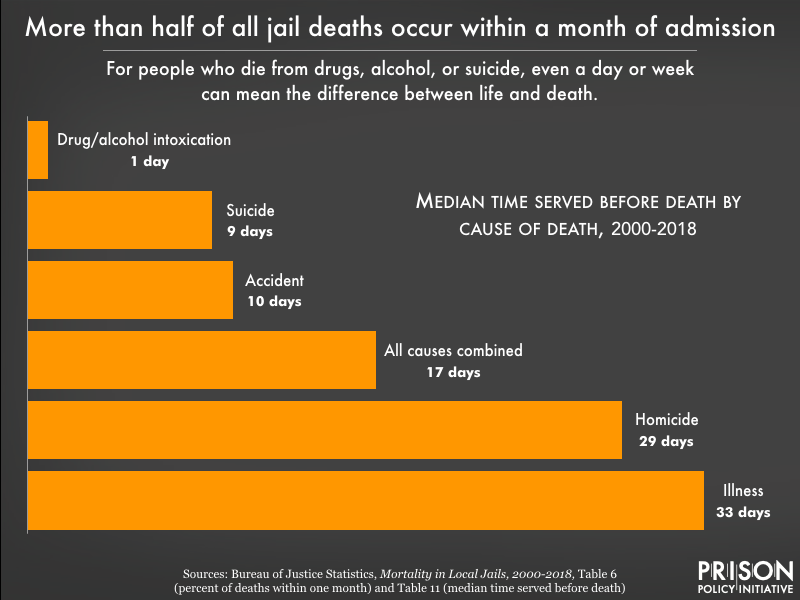
As in past years, suicide was the single leading cause of death for people in jails, accounting for almost 30% of deaths. Someone in jail is more than three times as likely to die from suicide as someone in the general U.S. population (and still twice as likely when the population is adjusted for age, sex and race/ethnicity to match jail populations).
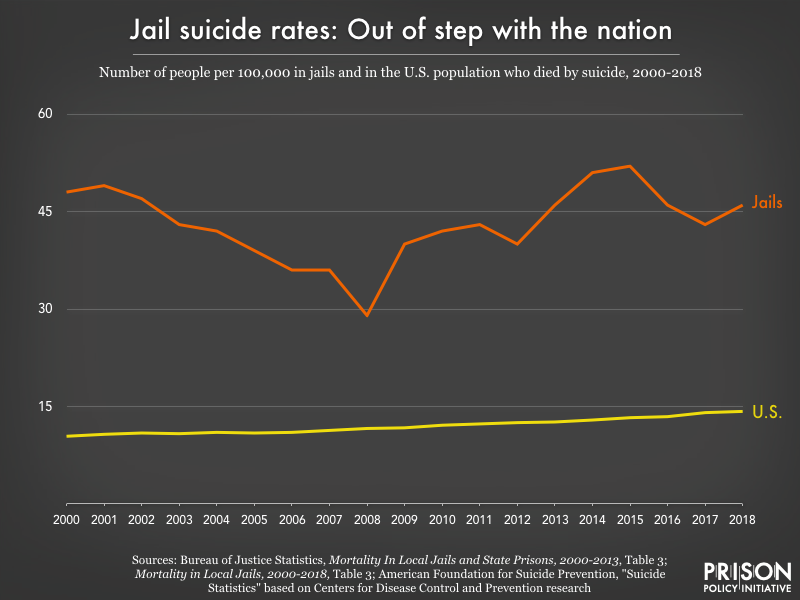
Suicide in jail tends to happen quickly: half of all those who died by suicide between 2000 and 2018 had been in jail for 9 days or less – compared to a median stay of 17 days for all causes of death. A short stay in jail can be extremely harmful, a fact that even our nation’s top officials acknowledge, noting that “certain features of the jail environment enhance suicidal behavior.”1 For suicide and deaths linked to drugs or alcohol, it’s those first few days in jail that are deadliest.
Millions of people are booked into jails each year with alcohol or drug use disorders, and the number who died of reported intoxication while locked up reached record highs in 2018. Since 2000, these deaths are up 381 percent, and over the entire 18 years of data collection, the median time served before a drug or alcohol intoxication death was just 1 day. One Texas woman, for example, was jailed for unpaid traffic tickets and died after 3 days from complications of withdrawal after begging for medical care, and instead, being asked to clean up her own vomit. With 18 years of data showing that jailing people with substance use disorders for low-level offenses so often leads to death, why are we still using jails as de facto detox facilities?
More women are entering – and dying in – jail
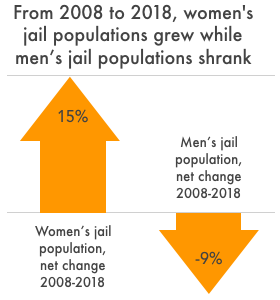
Women made up one-sixth of all jail deaths in 2018, slightly more than their share of the total jail population. Women also had a 7% higher mortality rate than men in jails; this isn’t the first year that was true, but because women are a key driver of jail population growth, the rise in their mortality rate should send correctional leaders and policymakers running toward solutions aimed at keeping women out of confinement.2
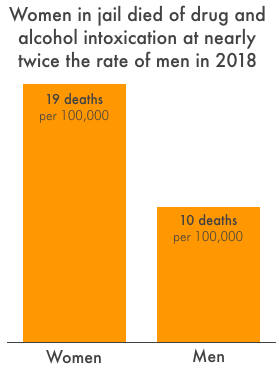
Previous research offers solid clues as to where to begin addressing the over-incarceration and preventable deaths of women. Between 2000 and 2018, women in jail died of drug and alcohol intoxication at twice the rate of men. (In state prisons, women died this way at half the rate of men.)3 Women are also more likely than men to enter jail with drugs in their system, with a medical problem or chronic condition, or with a serious mental illness.
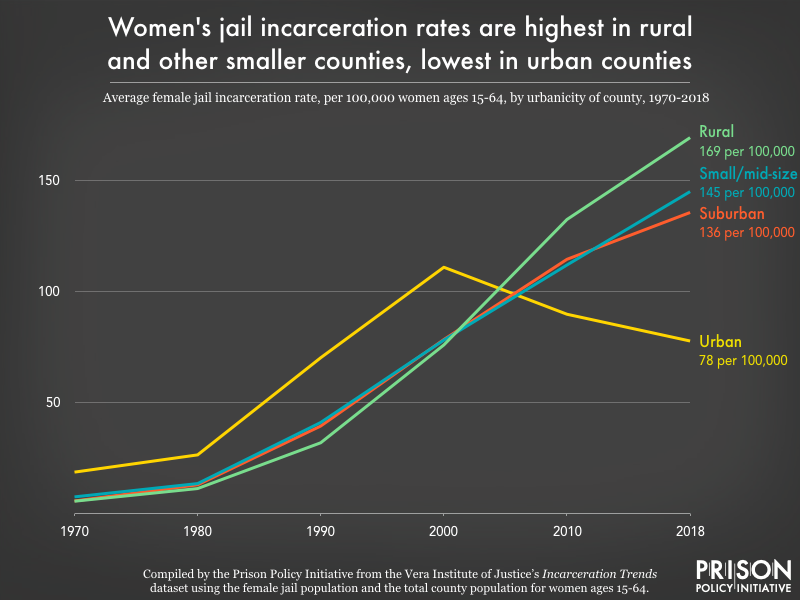
Rural jails, a growing force, had the highest death rates in 2018
Small jails – particularly those with an average daily population of 49 or fewer people – reported the highest mortality rates again in 2018. A long-standing reality, the mortality rate in these smallest jails has actually been more than double the overall jail mortality rate in some years. By absolute numbers, these deaths make up a small portion of all jail deaths each year, but rural areas have become major players in jail incarceration.4
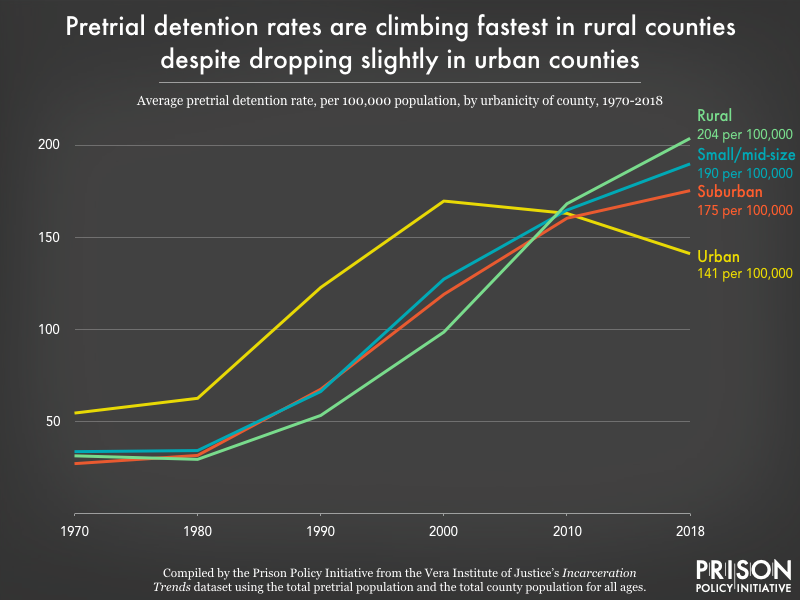
And yes, women and rural jails are growing together. Between 2004 and 2014, the number of women in jail increased 43 percent in rural counties, while declining 6 percent in urban counties. For decades, jails in non-urban jurisdictions have quietly proliferated, fueled by increases in pretrial detention. Additionally, researchers have found that women entering rural jails are significantly more likely to have co-occurring serious mental illness and substance use disorder, despite being severely under-identified by their jails as having such needs.
Jail healthcare is sketchy at best, and deadly at worst
But what does the growth of women’s jail populations across America have to do with mortality? In 2020, Reuters published an unsparing 3-part investigation of jail healthcare systems, deaths, and the increasing presence of women entering and dying there. Reporters established a devastating pipeline of women being arrested, locked up, and left to detox, give birth, or go without necessary psychiatric care in jail cells.
According to the report, on average, deaths were higher in those jails with privately contracted healthcare services, and rural jails are likely to go the private healthcare route.5 These companies’ profit motives shine through in haunting examples of neglect. At a Georgia jail managed by Corizon – a major private correctional healthcare company – senior leadership routinely overrode the recommendations of medical staff; patient names or prescription orders were simply removed from lists to avoid the bad optics of providing untimely care. But when counties move to end their healthcare contracts, there are few real competitors.
The idea that jails are falling short in their care sometimes fuels short-sighted arguments for expanding or building new facilities. One county in Texas was considering a new women’s facility in order to provide “gender-specific” and “trauma-informed” services to this population; fortunately, county commissioners recently postponed the vote to approve its construction at the suggestion of local activists and the county judge. These myopic projects are expensive and do not help communities – in fact, research shows that jail incarceration drives deaths within those counties.
Jails are shameful replacements for key social and medical services, and too often low-level offenses are used to justify locking people up, out of sight, when they simply need help. For women, “gender-responsive” strategies for diversion and treatment do exist, but policymakers should exercise caution in implementing those that are simply new forms of supervision; these programs will only increase the footprint of the criminal justice system. Decriminalization and the provision of gold-standard medical care, followed by a halt to jail construction, should be top of mind when addressing record mortality in jails; our mass incarceration crisis is troubling enough when people survive.
Footnotes
-
The Bureau of Justice Statistics plans to publish detailed data on suicide in U.S. correctional facilities in August 2021; the most recent version of this report is from 2002. ↩
-
Not only has the number of incarcerated women increased 14-fold from 1970 to 2014, but women are now found in jails in nearly every county in the US, whereas they were only found in about one-fourth of jails back then. This trend is so troubling, we made a Whole Pie focused on women’s mass incarceration. ↩
-
The Reuters investigation obtained jail mortality data through 2019, one year beyond what BJS published, and found that drug and alcohol-related deaths among women in jails has not subsided. From 2017 to 2019, about one-fourth of female deaths were linked to drugs or alcohol, compared to just one-eighth of deaths from 2008 to 2016. Still, both of these percentages were double those of men’s drug- and alcohol-related deaths. ↩
-
In one sense, rural jails and deaths receive lots of attention in local news and cultural commentary. In another, policy and research have largely focused on large urban jails and overlooked the complex needs of rural jails. General issues faced by rural jails and their surrounding communities include: an insufficient tax base to support adequate medical or social services, a serious shortage of lawyers and public defenders, and a dearth of general criminal justice system administration, from court hours of operation, to machinery, to investigators. ↩
-
Jails are not held to any national standard of healthcare, private or public, but can seek optional accreditation. The National Commission on Correctional Health Care offers accreditation to jails, prisons and other detention centers, but does not publish a full list of accredited facilities “by policy.” ↩