COVID-19 spread faster in counties with large prisons — and to nearby counties:
Marion Correctional Institution (Ohio) is a disturbing example
by Gregory Hooks
December 2020
As COVID-19 spread throughout the United States in the spring and summer of 2020, it was apparent that many prisons and jails were becoming virus hotspots. Less obvious was the fact that correctional institutions had become vectors of the virus, contributing to outside spread throughout the community and nearby areas. My analysis in the report Mass Incarceration, COVID-19, and Community Spread led me to estimate that prisons and jails were linked to an additional 566,804 COVID-19 cases throughout the United States from May 1st to August 1st.
To better illustrate the methods used in this analysis, here we take a closer look at Marion County, Ohio, where a multicounty jail and two state prisons are located, including Marion Correctional Institution (MCI), the site of one of the largest outbreaks of COVID-19 in the U.S. MCI illustrates how COVID-19 can spread rapidly among incarcerated people and prison staff, throughout a county, and on to surrounding areas.
Ohio — like the rest of the country — has fully embraced mass incarceration. Ohio’s prison population has tripled since 1980, and its overcrowded prisons held about 50,000 people at the end of 2019, despite having an overall capacity of less than 40,000.1
At the beginning of April, the state of Ohio reported a modest COVID-19 caseload, following aggressive steps by Gov. Michal DeWine to slow the spread of the virus. It was becoming abundantly clear, however, that infections were spreading rapidly among those incarcerated and working at MCI. When Ohio undertook systematic testing in its state prisons beginning April 11, nearly 4,000 incarcerated individuals tested positive for COVID-19. MCI accounted for more than half of these infections. The following table summarizes the remarkable outbreak at MCI and its prominence within the county and the state.
| Confirmed COVID-19 cases in: | MCI as percentage of total COVID-19 cases in: |
||||
|---|---|---|---|---|---|
| Date | MCI (prison) | Marion County | Marion County | State of Ohio | |
| April 1 | 0 | 9 | 0.0% | 0.0% | |
| April 8 | 0 | 32 | 0.0% | 0.0% | |
| April 15 | 0 | 164 | 0.0% | 0.0% | |
| April 22 | 2,011 | 2,137 | 94.1% | 14.2% | |
| April 29 | 2,011 | 2,196 | 91.6% | 11.6% | |
In late April, due to the prevalence of COVID-19 among those incarcerated in MCI, Marion County had the second-highest infection rate of any county in the United States. In fact, this single prison accounted for over 14% of the state’s entire caseload on April 22, and nearly 12% on April 29 (as testing capacity was expanding). All of Ohio’s prisons, taken together, contained 20% of the state’s known COVID-19 cases on April 20.
But as the Marion Star noted, a “prison outbreak doesn’t stop at the prison doors. It impacts the corrections officers and by extension, the communities they live in.” By April 20, more than 150 MCI employees had tested positive for COVID-19, and one staff member died as a result of the virus. COVID-19 infections linked to MCI were found in non-staff members in the Marion County population. And since a number of MCI staff, vendors, and visitors lived, worked, shopped, and visited in nearby counties, MCI-linked cases were found in nearby counties as well.
MCI provides a disturbing example of viral spread between the prison and community. But due to over-incarceration, MCI is just one of many large, crowded prisons and jails dotting the U.S. landscape. My study aimed to determine whether the community spread from the prison that was observed in Marion County was in fact a broader problem experienced by communities with large incarcerated populations nationwide.
To investigate the possibility that local incarcerated populations contributed to community spread of the pandemic, I conducted statistical analyses (explained in detail in the Methodological Appendix [PDF]) using the following two measures:
Measure 1: Incarcerated population density in each county:
According to the most recent Census data available, there were 4,749 people incarcerated in Marion County, which places the county in the top 10% of all U.S. counties by total incarcerated population. And with an incarcerated population density of 11.75 incarcerated people per square mile, Marion County also falls in the top 5% of U.S. counties when considering the population density of incarcerated populations.2
I estimate that incarceration within Marion County was responsible for an additional 310 COVID-19 cases in the county between May 1 and August 1 — or 37% of the county’s total cases during that period.
Marion was not an outlier in this respect. In my nationwide analysis, I found that in nonmetro counties across the country (like Marion County), high incarcerated population density had a significant impact on the county’s COVID-19 caseloads.
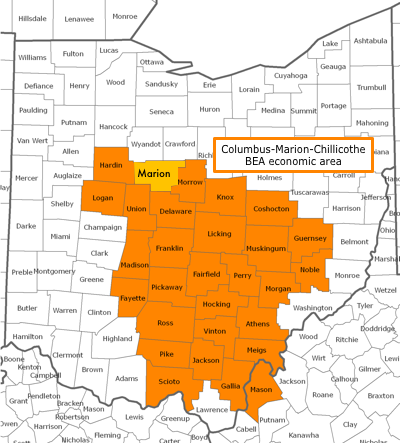
Measure 2: Incarcerated population density in the multicounty BEA economic area in which the county is located (excluding people incarcerated in the county itself):
Because COVID-19 does not respect county boundaries, I wanted to see whether infection rates were higher in counties that are located near other counties that house large prison and jail populations - as observed in those near Marion County. For this, I defined “other nearby counties” as being in the same BEA economic areas — clusters of counties that are economically linked through commuting patterns and media markets.3
For each county in the United States, I created a BEA area-level measure of the incarcerated population in the surrounding counties, by adding up all incarcerated people in the county’s BEA area, and then subtracting the number incarcerated within the particular county being studied. Again, I converted this to a measure of incarcerated population density, by dividing the incarcerated population by the number of square miles in the BEA area. This BEA area-level analysis allowed me to measure the impact that incarceration in nearby, economically linked counties had on a given county’s COVID-19 cases — separating this dynamic from the impact that a county’s own incarceration had on its COVID-19 caseload.
| County | BEA Economic Area | ||||||
|---|---|---|---|---|---|---|---|
| County | Incarcerated population in county | Area (square miles) | MEASURE 1: Incarceration density in county (persons per square mile) | Total incarcerated population in BEA area | Incarcerated population excluding county (BEA area total minus people incarcerated in county) | MEASURE 2: Incarceration density in the BEA area (persons per square mile)* | |
| Delaware | 195 | 457.3 | 0.43 | 32,379 | 32,184 | 2.35 | |
| Franklin | 2,353 | 543.5 | 4.33 | 32,379 | 30,026 | 2.20 | |
| Marion | 4,749 | 404.1 | 11.75 | 32,379 | 27,630 | 2.00 | |
| Ross | 5,647 | 693.0 | 8.15 | 32,379 | 26,732 | 1.98 | |
| Scioto | 1,695 | 616.2 | 2.75 | 32,379 | 30,684 | 2.26 | |
Among these five counties, Marion County has the highest incarceration density at the county level (11.75), but one of the lowest at the BEA area level (2.00). Delaware County, on the other hand, has the fewest people incarcerated (195) and lowest incarceration density at the county level (0.43). However, when calculating the comparable measure at the BEA area level for Delaware County, there are relatively few incarcerated people to subtract from the BEA area total, leaving the county with the highest measure of BEA area incarceration density (2.35). In this sense, the BEA area-level measure of incarceration density assesses the degree to which counties with relatively few people in jails and prisons faced heightened exposure to the novel coronavirus due to incarceration in nearby counties.
Unsurprisingly, the county-level analysis matched what local news outlets reported about Marion County — incarceration within Marion County (including at MCI) did contribute significantly to the county’s community spread. But my BEA area-level analysis further found that incarceration in the rest of the Columbus-Marion-Chillicothe BEA area also contributed to the spread of COVID-19 in Marion County. Incarceration in the surrounding BEA area added an estimated 144 COVID-19 cases to Marion County’s total between May 1 and August 1 — 13% of total cases in that timeframe — excluding the effect, discussed above, of Marion County’s own incarceration numbers.
This inter-county spread means that even counties with very little incarceration can feel the effects of incarceration-linked COVID-19 spread. Delaware County, which is also in the Columbus-Marion-Chillicothe economic area, houses just 195 incarcerated people (0.43 per square mile). Despite this low level of incarceration within Delaware County, I estimated that high incarceration in the other counties in the same BEA area was responsible for an additional 188 COVID-19 cases in Delaware County between May 1 and August 1 — amounting to 21% of the county’s total cases in that timeframe.
The trend in the Columbus-Marion-Chillicothe economic area held true throughout the country. Counties located in BEA economic areas with high levels of incarceration saw quicker growth in COVID-19 infections throughout the summer of 2020, even if these counties themselves did not have high levels of incarceration. For a full account of this study and its findings, see Mass Incarceration, COVID-19, and Community Spread.
Read more about the data
For details about the data sources and methodology, see Mass Incarceration, COVID-19, and Community Spread: Methodological Appendix [PDF] by Gregory Hooks.
About the Prison Policy Initiative
The non-profit non-partisan Prison Policy Initiative was founded in 2001 to expose the broader harm of mass criminalization and spark advocacy campaigns to create a more just society. It sounded the national alarm about the threat of coronavirus to jails and prisons with its March 2020 report No need to wait for pandemics: The public health case for criminal justice reform. The organization’s data-driven coverage of the pandemic behind bars continues to advance the national movement to protect incarcerated people from COVID-19.
About the author
Gregory Hooks is Professor of Sociology at McMaster University. In several prior works, he has examined the impact of prisons on local employment trends. This research raised doubts about the purported economic benefits of prisons. In fact, this research suggested that prison towns are at risk of ending up with a net decrease in jobs. For details on this line of research, see:
- Genter, Shaun, Gregory Hooks, and Clayton Mosher. 2013. Prisons, Jobs and Privatization: The Impact of Prisons on Employment Growth in Rural U.S. Counties, 1997-2004.
- Hooks, Gregory, Clayton Mosher, Shaun Genter, Thomas Rotolo and Linda Lobao. 2010. Revisiting the Impact of Prison-Building on Job Growth: Education, Incarceration and County-Level Employment, 1976-2004.
- Gregory Hooks, Linda Lobao, Clay Mosher, and Thomas Rotolo. 2004. The Prison Industry: Carceral Expansion and Employment in U.S. Counties, 1969-1994.
His research program examines spatial inequality broadly, including research into inequality and social policy, environmental inequality (from both military and civilian sources), and peace, war and development.
Footnotes
Ohio’s Department of Rehabilitation and Correction has not reported the state prison system’s capacity information to the federal Bureau of Justice Statistics since 2015. In a 2020 ProPublica article, ODRC spokesperson JoEllen Smith gave this explanation: “the design of a facility 60 years ago is not meaningful today due to the changing nature of the population.” The most recent available capacity information (from 2015) for the state’s prisons was 34,986, and the most recently reported capacity of its two private prisons was 4,738 (1,820 at Lake Erie Correctional Institution according to its PREA audit report published in April 2019, and 2,918 at North Central Correctional Complex according to its website in November 2020). The total population for all facilities was 48,732 on December 31, 2019, according to a weekly population count report ↩
- I chose to use population density as a measure of local incarceration because research into the spread of COVID-19 has highlighted the possibility that population density can play an important role. As these researchers have made clear, population density, in and of itself, does not facilitate the spread of the novel coronavirus. But where public health policies fail, population density amplifies these failures. In the case of mass incarceration, the profound and far-reaching failures in managing COVID-19 in prisons and jails have been well-documented. The consequences of these failures are amplified where the number of incarcerated persons per square mile is high, and diluted in places where incarcerated population density is lower.
The emphasis that BEA economic areas place on commuting makes these geographies well-suited for this analysis of “community spread” related to prisons and jails across a multicounty area. Those who work in one county but live in another county are exposed to the novel coronavirus in more than one county, and if they become infected, they can infect people in more than one county. ↩
Events
- July 1, 2026:
On July 1, 2026 at 1 p.m. EST, join the Prison Policy Initiative and guests Jodi Hocking, Executive Director of Return Strong Nevada, and Taj Mahon-Haft PhD, Director of The Humanization Project, as they discuss the importance of family connections, highlight the ways they are under attack, and share strategies to help families fight back.
Register here
Not near you?
Invite us to your city, college or organization.